A 20-year journey of health research: Quantifying a rural network
19 May 2021

Dr. Martha MacLeod. Photo credit: Northeast News. Photo courtesy of Martha MacLeod
Dr. Stefan Grzybowski. Photo credit: Vancouver Coastal Health Research Institute
Drs. Stefan Grzybowski and Martha MacLeod: Quantifying a rural network
It was 2005 and it wasn’t immediately apparent to Dr. Stefan Grzybowski and the small team meeting over a conference call that they would be part of a new initiative to build partnerships among rural and remote BC researchers. But they would soon learn that MSFHR intended to provide seed funding for the network that would spark further developments for rural and remote health research.
“It happened almost organically,” Stefan says about the early days of the BC Rural and Remote Health Research Network. “And then we became a bit of an incubator.”
With a focus on building future capacity for health research in BC, between 2004 to 2010 MSFHR funded eight Health of Population Networks to build partnerships among BC researchers conducting research related to specific population groups. One of these networks was the BC Rural and Remote Health Research Network, co-led by Dr. Grzybowski, a family physician with many years of rural clinical experience, and Dr. Martha MacLeod, a UNBC-based researcher and long-time supporter of and advocate for improving the health of rural and remote populations.
“There is a way of working with rural, remote and northern communities on research that spans both Western and Indigenous ways of knowing and learning. Everyone has to learn it when they get here. You have to be invited to the community and have that ongoing commitment to partnership.”

In the initial MSFHR funding application for the BC Rural and Remote Health Research Network, it was noted that there is substantial evidence that rural, remote and northern populations experience compromised health status when compared to their urban counterparts. This experience is understood all too well by health researchers based outside of BC’s urban areas. Martha remembers working alongside several other UNBC faculty members and researchers in a small office in downtown Prince George, together fostering new connections for rural researchers across Canada. There were a number of rural health research endeavours just getting started, and she was excited to build capacity for research partnerships and turn away from the data extraction models of the past.
“Innovation often happens at the margins,” she explains. “There is a way of working with rural, remote and northern communities on research that spans both Western and Indigenous ways of knowing and learning. Everyone has to learn it when they get here. You have to be invited to the community and have that ongoing commitment to partnership.”
With funding from MSFHR, Stefan, Martha and their team focused their efforts on building up the rural and remote health research community to allow for greater knowledge sharing.
Stefan points to the development of the team awards by the BC Rural and Remote Health Research Network as one of the most successful strategies that pulled groups of people together and helped expand further networking and connections among BC’s rural and remote researchers. Many of the teams that received support from MSFHR were able to apply for and receive further funding and grants from larger national organizations like CIHR to continue their research.
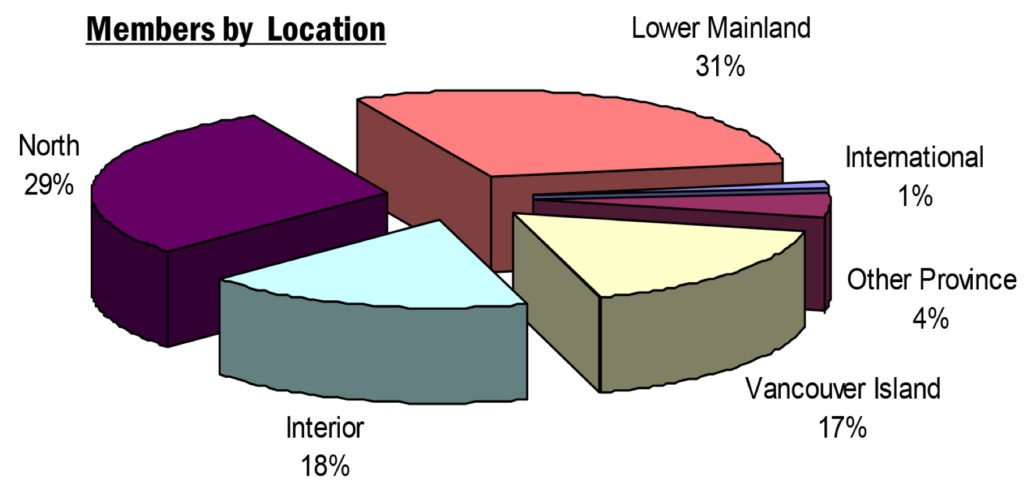
Stefan credits MSFHR for its contributions to investigating and clarifying the unique challenges of rural health research. The difference between urban and rural health research is clear: while urban centres allow for specialization, rural research needs to recognize generalist ways of approaching problems.
Some of his latest health research focuses on challenges for maternity care in rural areas and demonstrates the impact of these challenges on families and communities. While there are several factors that affect the delivery of maternity care in rural areas, in one research example, Stefan’s team evaluated if having access to a physician who can perform surgeries would affect the number of women who chose to deliver at their local hospital. This focused rural health research allows for local and surrounding health areas to better understand the impact of their service delivery and reveals opportunities for quality improvement to better serve community members in other catchment areas.
“Different health systems weren’t well understood, and MSFHR contributed to unpacking and understanding some of that. I applaud MSFHR for their boldest vision and the large amount of resources they put forward to support health research across the province.”

Martha is still based at UNBC where she continues to advocate, create research knowledge opportunities and support their subsequent translation into practice across the province. She is also part of the Advisory Council for the BC SUPPORT Unit and is active at BC SUPPORT Unit Northern Centre, where she is currently exploring patient-oriented approaches to implementation science and knowledge translation. Both have also served on MSFHR peer review panels.
In looking back, Stefan remarks, “Different health systems weren’t well understood, and MSFHR contributed to unpacking and understanding some of that. I applaud MSFHR for their boldest vision and the large amount of resources they put forward to support health research across the province.”

A rural and remote network in action
Dr. Marina Morrow of Simon Fraser University was one of the first researchers to receive seed funding from the BCRRHRN for her research examining mental health service provision within northern and remote settings. More specifically, Dr. Morrow’s study Mental Health Reform: Understanding Rural Community Capacity identified the important factors impacting older adults needing mental health services who were either relocating from larger centres or aging in place.
The team concluded that building community capacity to deal with the complex needs of these patients was severely hampered not only by facility and regional health authority staff turnover, but also by the stresses inherent to working in northern communities, which include geographic, social and economic challenges. Their findings have since informed service planning in rural and northern BC.
Further, Dr. Morrow and her team went on to obtain funding through CIHR to establish the Centre for the Study of Gender, Social Inequities and Mental Health (CGSM), which has undertaken BC-wide research since 2009. Working with academic and community researchers, community service providers, policy-makers, practitioners, advocates and those who have experience with mental illness from across Canada, the U.S., the UK and Australia, the centre aims to create a better understanding of why disparities in mental health and addictions outcomes persist, so that appropriate programs, policies and interventions can be developed and implemented.
Learn more:
MSFHR 2005 Health of Population Networks Award: BC Rural and Remote Health Research Network
MSFHR 2005 Investigative Team Award: Rural and Northern Practice and its Development
Rural Health Services Research Network of BC (Formerly BC Rural and Remote Health Research Network)
New Rural Health Research Network Launched at UNBC (UNBC, July, 2005)
Canadian Rural Health Research Society: Creating Capacity Through Connection (March, 2007)
MSFHR Researcher Profile and List of Publications: Dr. Stefan Grzybowski