Rooted in relationships: Lessons learned from Indigenous health researchers and community members
11 June 2024

Photo: Leaders supporting the Indigenous Health Research Ethics in Clinical Research Symposium. Left to right, top to bottom: Dr. Jeffrey Reading, Dr. Stirling Bryan, Dr. Krista Stelkia, Mark Matthew, Gillian Corless, Dr. Evan Adams, Tara Erb.
What you should know
|
|---|
What is cultural safety in clinical health research?
Colonization and systemic racism have critically impacted the past and ongoing health and wellbeing of First Nations, Métis and Inuit Peoples. Evidence shows centuries of intentional and unjust research practices have harmed Indigenous populations. This includes research data being collected from Indigenous community members and used or disclosed without participants’ knowledge or consent. If health research does harm, what can help restore trust? What is cultural safety in health research, and how can we uphold cultural safety within health research environments?
Almost 100 people from across BC joined together to explore solutions. The Indigenous Health Research Ethics in Clinical Research Symposium was held on April 16, 2024 on the traditional, ancestral, unceded territory of the xʷməθkʷəy̓əm (Musqueam) people in Vancouver.
The symposium brought together Indigenous and non-Indigenous health researchers, trainees, community members and allies, along with research ethics leaders and representatives from health authorities and the Ministry of Health.
The symposium aimed to:
- deepen how Indigenous health research ethics is understood in clinical research;
- network, connect and provide mentorship; and
- support research talent development opportunities for Indigenous scholars, students and people beginning their careers.
Indigenous communities must lead health research
“Research is only as meaningful and relevant as it is useful to communities. Research should be led by us, for us, with us.” – Dr. Evan Adams, Tla’amin, deputy chief medical officer, First Nations Health Authority
During the symposium, presenters shared personal experiences, wisdom and best practices around Indigenous health research. Attendees learned that people and communities need to be engaged in health research. Indigenous rights and self-determination must be central to this work.
What does that mean for non-Indigenous researchers? Researchers need to be ready to let communities lead. Build relationships. Respect communities’ timelines and protocols. Be willing to listen and learn.
“You have to go in with a humble heart and recognize that you have as much to learn from communities as they have to learn from you,” says Dr. Pablo Nepomnaschy, professor at Simon Fraser University, speaking as an ally.
Community-led research is vital to support the leadership and self-determination of Indigenous peoples. One example of this work has been done through the relationship between the Nuu-chah-nulth Tribal Council and researchers at Simon Fraser University. Nuu-chah-nulth Tribal Council members developed an ethics protocol that engages 14 Nations in health research priority-setting.
“One person cannot speak for a whole community,” says Lynnette Lucas, Nuu-chah-nulth, health director, department of health, Nuu-chah-nulth Tribal Council. “So, we had to talk to traditional leaders, elected and hereditary leaders, heads of households, professionals. You need to develop these relationships along the way. That’s how you make sure research is truly community-led.”
Redefining research success
However, it isn’t enough to change how researchers engage with Indigenous communities. Institutions, such as universities and research funding bodies, also need to adjust processes, timelines and policies.
For example, institutions can change how research success is defined, to include not only the number of academic articles, but also relationship building. Similarly, funding bodies may expand the types of institutions that can hold funds.
“Universities need to focus on their own systems and structures. It’s hard to do this work if there is no change,” says Tara Erb, Moose Cree, network coordinator of the BC Network Environment for Indigenous Health Research (BC NEIHR).
Indigenous values should ground research
Indigenous values should ground research. Two environmental scans led by Indigenous health researchers provide guidance and best practices.
An environmental scan of 21 research ethics boards in BC showed that many were unaware of formal ethics processes in Indigenous communities, collectives and organizations (ICCOS). This means that research ethics boards need infrastructure to engage with ICCOs as well as Indigenous researchers. This will help research ethics boards who are trying to respect Indigenous self-determination in research.
An environmental scan of Indigenous health research and evaluation practices shared protocols from across BC. This scan strengthens and acknowledges decolonized Indigenous engagement practices for researchers to begin engaging with communities in a culturally safe way.
Resources like these call for systems change and increased Indigenous self-determination in health research systems.
Research partnerships are rooted in relationships
“Better relations open the doors to many things.” – Elder Dave Frank, Ahousaht
“The symposium demonstrates the continued partnership of the BC SUPPORT Unit and the BC Network Environment for Indigenous Health Research,” says Monica Mamut, director, BC SUPPORT Unit. “We’re grateful to continue working together in a good way.”
The BC NEIHR is one of nine Indigenous-led networks across Canada that support research leadership among Indigenous (First Nations, Métis and Inuit) communities, collectives and organizations. BC NEIHR is funded by the Canadian Health Research’s Institute of Indigenous Peoples’ Health.
The BC SUPPORT Unit moves evidence developed with patients and communities into practice. This provincial initiative is founded under Canada’s Strategy for Patient-Oriented Research. The BC SUPPORT Unit is part of Michael Smith Health Research BC and is funded by the provincial and the Canadian Institutes for Health Research. Symposium partners also included the Centre for Collaborative Action on Indigenous Health Governance and Research Ethics BC, also a part of Health Research BC. Together, these organizations are helping centre Indigenous ways of knowing in health research.
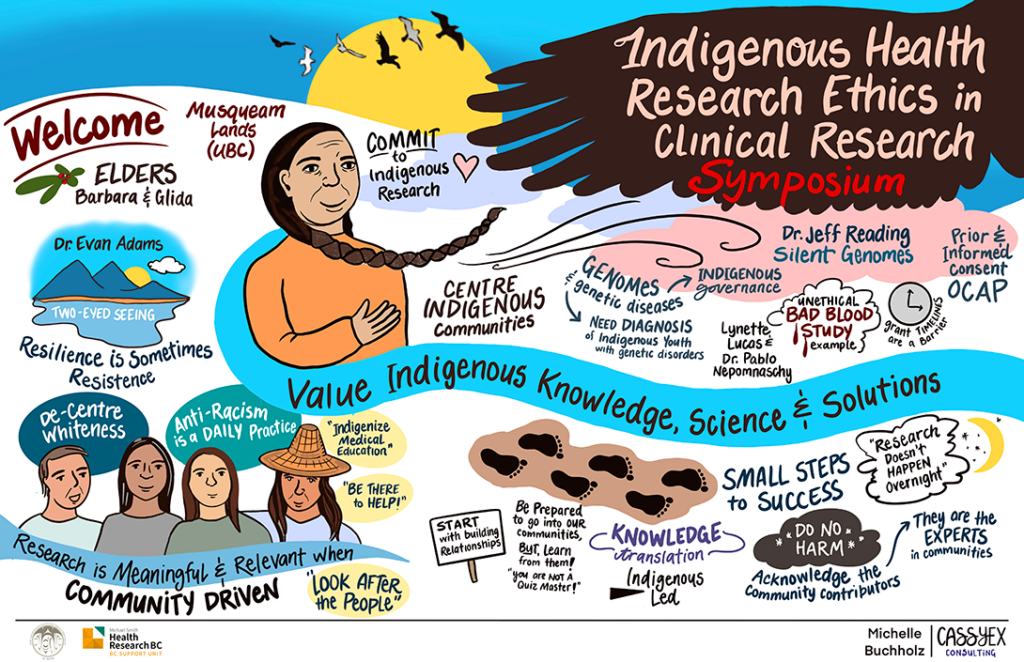
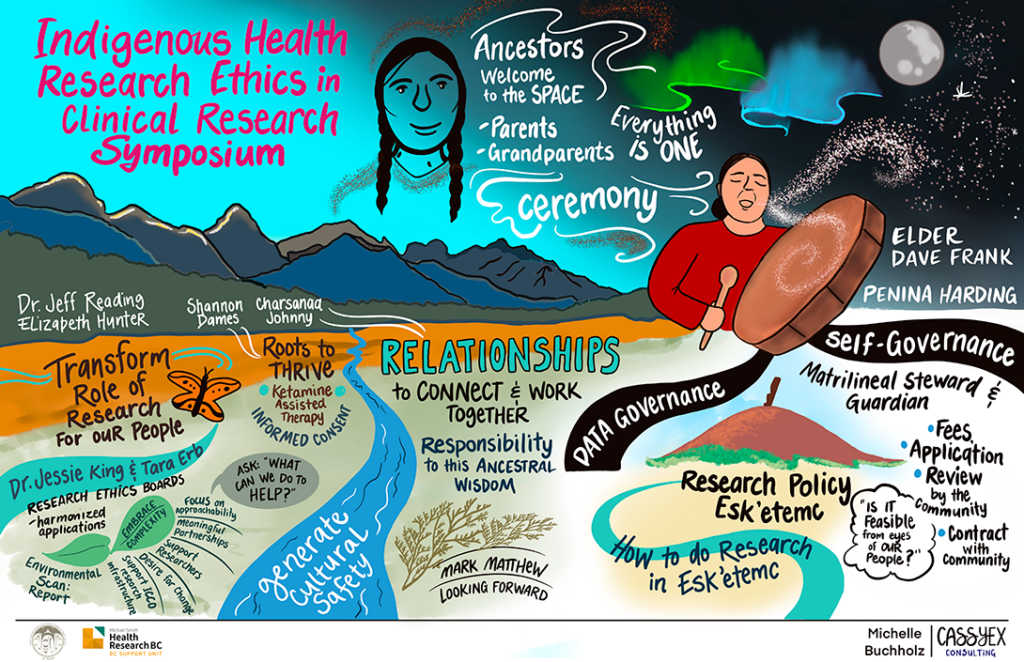
Graphic recording by Michelle Buchholz at Cassyex Consulting





