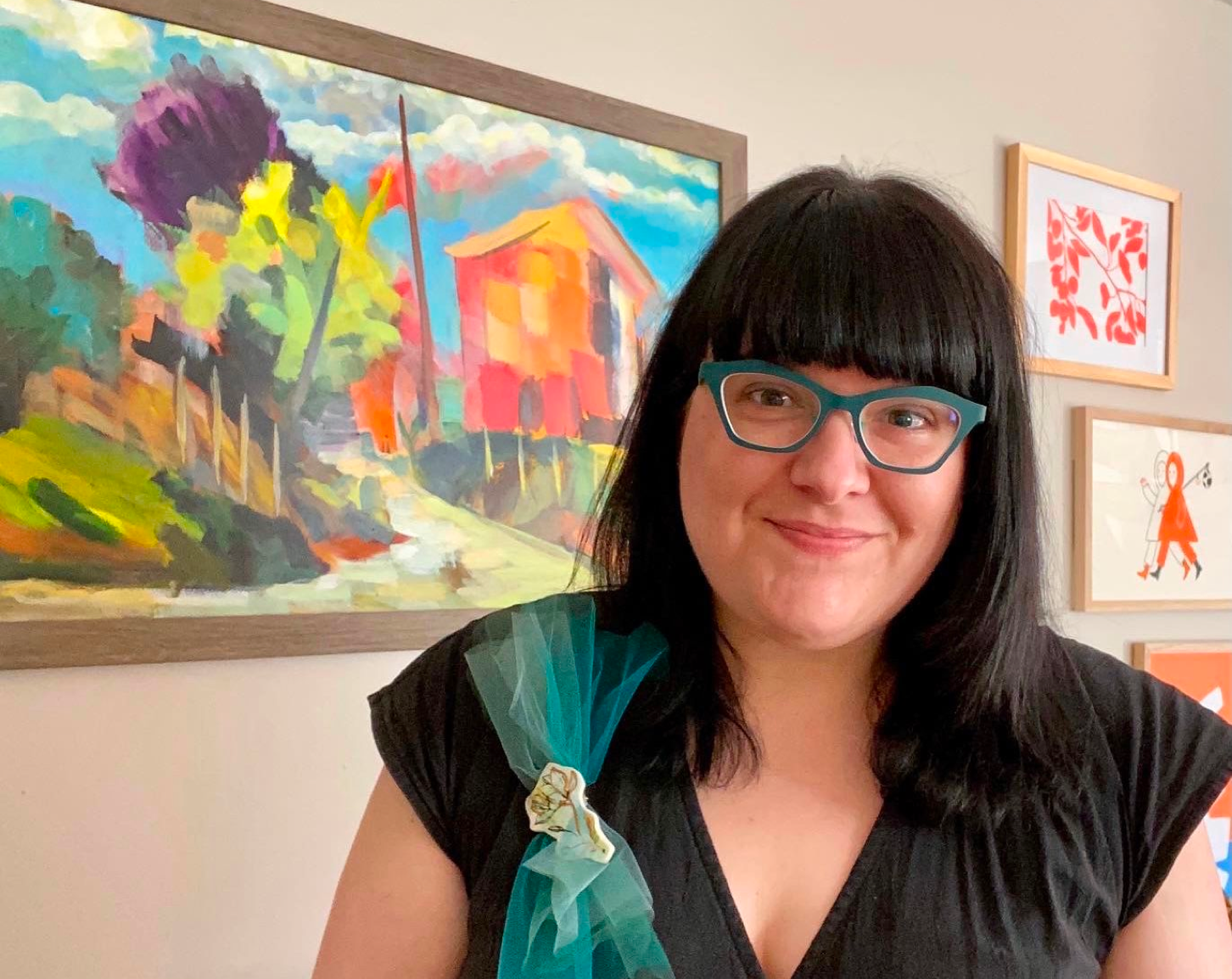A 20-year journey of health research in BC: Tackling emerging disease threats through rapid response research
9 June 2021

Dr. Danuta Skowronski, Epidemiology Lead of Influenza & Emerging Respiratory Pathogens at the BC Centre for Disease Control. Photo credit: The Star
Dr. Danuta Skowronski: Tackling emerging disease threats through rapid response research
It’s an approach more commonly associated with security teams: detect the threat and efficiently mobilize teams to characterize and mitigate the risk. For Dr. Danuta Skowronski, this is the approach that she and her team routinely take to inform the public health response to emerging diseases with pandemic potential, such as influenza viruses (like the cause of the 2009 H1N1 pandemic) or coronaviruses (such as SARS in 2003 and the current COVID-19 pandemic).
The long-standing Epidemiology Lead of Influenza & Emerging Respiratory Pathogens at the BC Centre for Disease Control (BCCDC), Danuta guides her team in conducting rapid response research necessary to address an emerging or evolving communicable disease crisis. Characterizing the features (i.e. epidemiological, virological, molecular and immunological) of animal-origin disease threats is critical to informing how to contain them or what countermeasures to use. This information helps understand whether vaccines can be helpful against the threat, and, if so, how quickly an immunization campaign is needed. This process requires efficiency, experience and expertise, and includes multi-disciplinary collaborations that support a public health mandate.
As Danuta describes it, one year of working on her intense and immersive team during a pandemic is equivalent to five to 10 years of concentrated learning and discovery. “It’s still exciting even after 20 years,” she says. “Prevention is key to staying ahead of the curve and that’s critical to protecting public interest. Moreover, our preliminary findings have immediate relevance and impact: people are always knocking on the door to learn what we know as soon as we know it, so the team has to be trained to be ready, set, go.”
Danuta’s introduction to rapid response research began in 2000 when she was part of the team investigating an unexpected “safety signal” associated with the influenza vaccine at the time. Symptoms of what became known as oculorespiratory syndrome varied from mild to severe, including red eyes to difficulty breathing. It became a race against the clock to understand the cause and severity of this syndrome to inform the benefits and risks of the ongoing immunization campaign that season. Her work in collaborating with national partners led to improvements in vaccine monitoring and manufacturing, and informed recommendations for the safe re-immunization of those affected.
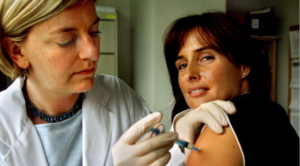
Photo credit: Chuck Stoody, The Canadian Press
In the years that followed, Danuta supported several major public health research and response teams, including the successful containment of SARS in 2003 in BC; the largest avian influenza outbreak in Canadian history (due to H7N3) in the Fraser Valley in 2004; and other emerging influenza variant risk assessments. The thrill of making discoveries that have had a real impact on individuals and whole populations has motivated her to continue her exhaustive work on emerging pathogens.

In mid-2008, Danuta hired two new epidemiologists, Dr. Naveed Janjua and Dr. Travis Salway, to her Influenza & Emerging Respiratory Pathogens team at the BCCDC. These were timely hires that enabled more support for the team’s critical work — the following April, the H1N1 virus emerged. In their very first season working on influenza, her new team members were confronted by a pandemic.
Contrary to typical seasonal influenza, H1N1 occurred in greater numbers in younger people than in those 65 years old. With funding from MSFHR and the Provincial Health Services Authority, Danuta led her team in understanding why older adults were relatively spared during the 2009 pandemic. The team discovered that different age groups had different levels of pre-existing immunity to H1N1, even though it was considered a new virus (also known as a novel pathogen).
“Prevention is key to staying ahead of the curve and that’s critical to protecting public interest.”
Their pioneering work showed that the older generation had built immunity to another similar strain of the virus during a pandemic that had taken place between 1918 and 1930, and, decades later, this gave them the antibodies to fight off the H1N1 strain circulating in 2009. It was a discovery that re-opened discussions about “imprinting”: the durable impact of a person’s first exposure to the influenza virus in childhood and how it influences their response to influenza viruses, both novel and seasonal, for the rest of their lives.
In a separate research project, Danuta’s team showed how the immune system reacts to seasonal and pandemic viruses can also have implications for influenza immunization campaigns. Together, her team’s impressive research during the 2009 pandemic directly informed vaccine policy decisions that year and opened the field for future research to explore this “imprinting” phenomenon.
“Sometimes you don’t need a huge team, just dedicated and curious individuals who work well together.”
Danuta describes the experience her new team members have working on understanding emerging pathogens as a kind of boot camp for the brain. “The rapid response to fill in gaps of knowledge, of synthesizing emerging evidence during a dynamic crisis into a benefit assessment, and making recommendations that best serve the population is a big responsibility. If you ask any of my team members, they will tell you it’s high-intensity but thrilling work. It’s a quickstep march to knowledge generation and translation.”
With each influenza season, Danuta and her team refine their research approach, using available information such as genomics and immuno-epidemiological tools. It’s a responsibility she and her team takes seriously. Since 2004, Danuta’s team has provided the only mid-season influenza vaccine effectiveness monitoring in Canada — evidence she has submitted each year for the past five years to the World Health Organization to inform its annual vaccine strain updates that have led to further important insights into influenza vaccine improvements.

In December 2019, Danuta brought on a new team member; a timely hire that was eerily followed by COVID-19 being declared a pandemic by the World Health Organization in early 2020. Similar to the new hires brought on before H1N1 in 2009, the added resources became real assets in responding to both of these global disease threats. When the COVID-19 pandemic hit, Danuta received funding from MSFHR to support an urgent need to understand how the virus was showing up in the BC population. Among other research findings, her thought-provoking analyses on the safety and efficacy of the mRNA COVID-19 vaccine directly informed the recommendation to extend the time between the first and second doses of the COVID-19 vaccine to enable more people to benefit from the substantial single dose protection. This recommendation, which she made in BC during a period of scarce vaccine supply and heightened epidemic activity, was adopted nationally and likely prevented thousands of hospitalizations across Canada during the third wave of the pandemic. The test-negative design methods pioneered by Danuta in 2004 are now also being used globally, including in BC to monitor vaccine effectiveness against COVID-19, including variants of concern.
As one of the pre-eminent voices in influenza research and with many years of life-changing research under her belt, Danuta is most proud of the way she has been able to inspire each of her team members to go above and beyond in protecting public health. Naveed and Travis from her 2009 H1N1 team have gone on to lead other research projects, and she still keeps in touch with them. Naveed was a recipient of the MSFHR 2020 COVID-19 Research Response Fund award, and Travis received the MSFHR 2017 Trainee award and 2019 Scholar award. Supported by epidemiologists in the larger BCCDC departments and the Public Health Laboratory led by Dr. Mel Krajden, Danuta still rolls up her sleeves to work alongside her current team. “I now have a wonderful, hardworking, intelligent and diverse group of women on my team,” she says. “And I am so proud of them. Sometimes you don’t need a huge team, just dedicated and curious individuals who work well together. It warms my heart to see how hard they work and how inspired they have been to give their all during this COVID-19 pandemic.”
1 https://www.cdc.gov/flu/pandemic-resources/2009-h1n1-pandemic.html
Learn more:
BC Researchers Investigate H1N1 Risk Factors (MSFHR, September 2009)
H1N1 Lessons Inform Future Pandemic Response (MSFHR, May 2012)